Integrative Medicine Case Reports, Volume 4, Issue 2 (July), 2023
Efficacy of Yoga therapy as Non-pharmacological management in Women with High-risk Pregnancy: A Single Case Report
KEY WORDS |
ABSTRACT |
|
High-risk Pregnancy
|
This present case study is about a High-risk Pregnancy that includes Pregnancy-induced Hypertension and an abnormal range of Uterine artery pressure, 22 years old female consulted to Gynaecologist for a complaint of missing menstrual cycle. They were diagnosed with Pregnancy positive with the help of a urinary pregnancy test (UPT). In the 13th week, as per a routine follow-up gone for an antenatal ultrasound scan report shows a There is a single live intrauterine gestation with an abnormal range of Right uterine artery PI and left uterine artery PI and diagnosed as a high-risk pregnancy. After a week, time patient has given a blood sample for a thyroid profile. Reports revealed that TRI IODO THYRONINE (T3)-2.13H and THYROXINE (T4) 21.9 H are in the higher range and noticed blood pressure range in higher side diagnosed as Pregnancy induced Hypertension (PIH)High-risk pregnancy will affect both mother and fetus in its way, on mother side, it increases blood pressure called preeclampsia and affects fetal growth result in Intrauterine growth restriction, premature birth, Stillbirth. After the 13th week of Pregnancy diagnosed with high-risk Pregnancy, patients are introduced to yoga therapy, including Asana, Pranayama, Meditation, etc., for three days a week regularly till the date of delivery and followed case till delivery. Yoga helps normalize blood pressure and impacts pregnancy outcomes as a standard range of APGAR score in babies and healthy birth weight. It does not show any complications of High-risk Pregnancy on the maternal and fetal side.
doi: 10.38205/imcr.040256 |
|
*Corresponding Author:
|
Introduction
Pregnancy is a life-changing experience for women. Many changes occur in the female body physically, emotionally, and psychologically. Placenta is the first structure that forms between the mother and fetus. It is a connection or bridge to provide nutrition and oxygen to a fetus for its growth and development. A placental disease is any disease, disorder, or pathology of the placenta (1). The placenta starts organogenesis in the very early stage of embryogenesis, governs fetal growth, and terminates its fate immediately after delivery. Placental perfusion is maintained by two different cardiovascular systems, i.e., maternal blood flow and fetal circulation. Therefore, the pathophysiology of the placenta is closely associated with maternal status and fetal development (2) (Figure 1).

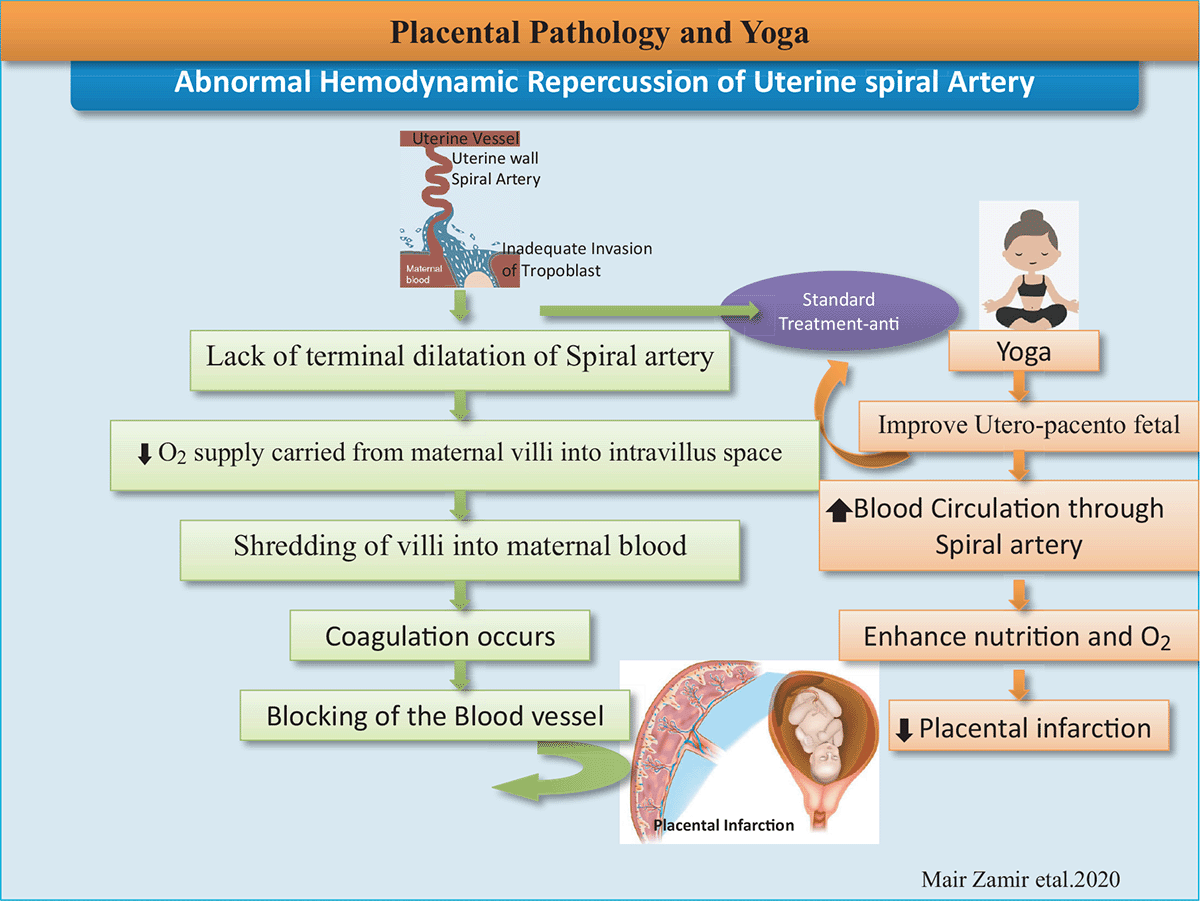
Figure 1: The diagram illustrates mechanism of Placental Pathology and effect of yoga intervention.
Placental disease/Pathology is abnormalities present within spiral arteries of the uterus. The terminal part of spiral arteries doesn’t dilate due to the lack of oxygen supply, carried from the maternal villa into Intravillus space, but because of lack of terminal dilatation in shredding of the villa into maternal blood, as such coagulation occurs resulting in the blockage of blood vessels leading to Placental infarction (3). The prevalence of placental pathology in low birth weight infants was 80.7%. The four types of placental pathology were related to low birth weight, Intrauterine Growth Restriction (IUGR), vascular anomalies of the deciduas, and Premature labour (4).
Approximately 800 women die during Pregnancy or childbirth every day (5). Obstetric hemorrhage (antepartum and postpartum), sepsis, and Hypertension during pregnancy accounts for more than 50% of maternal deaths worldwide, 99% of which occur in low- and middle-income countries (5). The World Health Organization estimates that approximately 15 million babies are born prematurely every year, and 1 million of these babies die despite the interventions that is capable of saving 75% of lives (6).
The overall estimated Still Birth Rate in the study population from the nine states in India was approximately half that of the WHO estimated rate of 22 per 1000 total births (7). It is observed that the Cesarean Section (CS) births increase with the advancing age of the women at the time of first delivery from 15.1% in ages less than 19 years to 53.2% of those over 35 is considered high-risk Pregnancy due to placental abnormalities. Women with high blood pressure during Pregnancy had a significantly higher proportion of CS births than those who had normal blood pressure (35.1% vs. 22.6%) (8).
Stillbirths and neonatal passing are worldwide issues, with more than 6.4 million passing happening yearly. An efficient survey presumed that pathology of the placenta, string, or layers is credited as a reason or contributory to stillbirth in 11% to 65% of cases in different orders, contingent upon the grouping utilized (3). The non-pharmacological techniques such as rest, music therapy, aromatherapy, relaxation therapy, acupuncture, acupressure, massage therapy, device-guided slow breathing, counselling, physical exercise, and yoga practice. That can potentially lower blood pressure among pregnant women with Hypertension and its complications. Mind-body therapy involves visualizing various mental images to facilitate relaxation and reduction in blood pressure (9).
Case Presentation
A primigravida 22 years female complained of a missing menstrual cycle and was diagnosed with Pregnancy positive with the help of a urinary pregnancy test (UPT). In the 13th week, as per a routine follow-up for an antenatal ultrasound scan, reports show that there is a single live intrauterine gestation. Right uterine artery PI 2.89 and left uterine artery PI 2.10. Mean PI 2.49 and diagnosed UAD positive as a high-risk pregnancy. After a week time, the patient has given a blood sample for a thyroid profile, and reports revealed that TRI IODO THYRONINE (T3)-2.13 H and THYROXINE (T4) 21.9 H are in the higher range and a blood pressure marked as 150/100 mm/hg diagnosed as a pregnancy induced Hypertension.
Discussion
Yoga therapy is vital to minimize complications related to High-risk pregnancies such as Pregnancy-induced Hypertension (Figure 2). Here is a case study that shows an abnormal range of uterine artery PI (Right and Left), is used to screen high-risk pregnancies with the help of a Doppler scan at 13 weeks of gestational age. Patient blood pressure indicates a PIH, as well as patients diagnosed with the abnormal range of thyroid profile during gestational age. Yoga therapy was administered to the patient after 12 weeks of Gestation, including Asana, Pranayama, Meditation (MSRT), and Yogic Relaxation techniques (Deep relaxation technique) practises (Table 1) that have been researched based and validated in the previous study (11).
Table 1: Intervention (10): 3 days in a week from 2nd trimester
| Yoga group | 2nd Trimester | 3rd Trimester |
| A. Lectures | 15 min | 10 min |
| B. Breathing Exercises | 10 min | 5 min |
| 1. (Hands in and out breathing) | Yes | Yes |
| 2. (Hands stretch breathing) | Yes | Yes |
| 3. (Ankle stretch breathing) | Yes | Yes |
| 4. (Tiger breathing) | Yes | Yes |
| 5. (Bridge posture breathing) | Yes | No |
| C. Asana Postures | 15 min | 10 min |
| 1. Tadasana (tree pose) | Yes | Yes |
| 2. Ardhakati-chakrasana (Lateral Arc Pose) | Yes | Yes |
| 3. Trikonasana (triangle pose) | Yes | Yes |
| 4. Vajrasana (The Ankle Posture) | Yes | Yes |
| 5. Vakrasana (spine twist pose) | Yes | No |
| 6. Siddhasana (sage pose) | Yes | Yes |
| 7. Baddha Konasana (Bound Ankle Pose)* | No | Yes |
| 8. Upavista Konasana (sit with legs apart)* | No | Yes |
| 9. Squatting (Garland pose)* | No | Yes |
| 10. Setubandhasana (Bridge posture) | Yes | No |
| 11. Viparitakarani (half-shoulder stand) | Yes | No |
| 12. Ardha-pavanamuktasana (folded leg lumbar stretch) | Yes | Yes |
| D. Pranayama & Meditation | 10 min | 20 min |
| 1. Sectional breathing | Yes | Yes |
| 2. Naadisuddhi (100 rounds) | Yes | Yes |
| 3. Sheetali, bharamari | Yes | Yes |
| 4. Nadanusandhana | Yes | Yes |
| 5. Om Meditation | Yes | Yes |
| 6. MSRT | Yes | Yes |
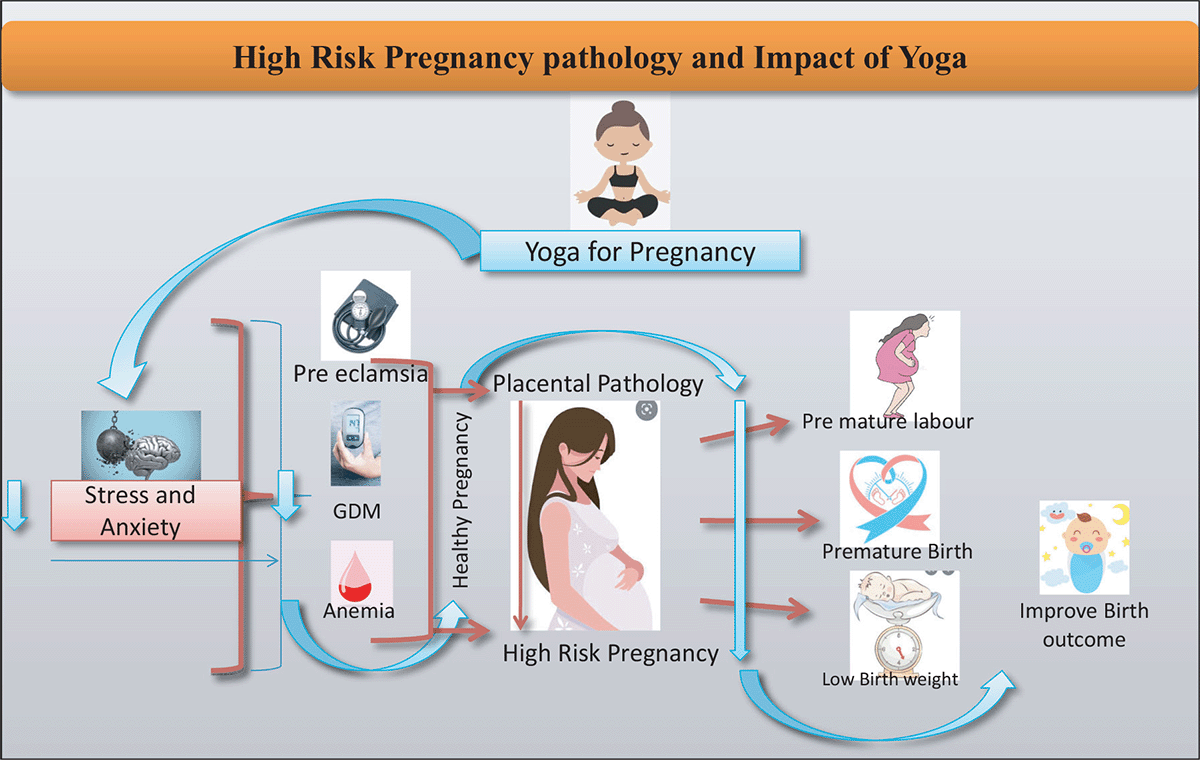
Figure 2: An overview of High-Risk Pregnancy and Impact of Yoga.
At 13 week of gestational age, Physiological parameters (Table 2) such as blood pressure and antenatal scan, including artery PI, shows an abnormal range. In contrast, after the intervention, an 18-week scan shows a standard range of uterine artery PI, indicating proper blood circulation and nutrition to the growing fetus. There marked a significant change in psychological parameters Perceived stress scale (PSS), Depression anxiety assessment scale (DASS), and Sleep quality as shown in (Figure 3) and (Figure 4).
Table 2: Parameters
| Parameters | 13 weeks of Gestation | 18 weeks of Gestation | 31 weeks of Gestation |
| Physiological variables | |||
| Blood pressure | 150/100 mm/hg | 140/100 mm/hg | 150/100 mm/hg |
| Pulse rate | 98 bpm | 96 bpm | 96 bpm |
| Physiological variables | |||
| GRAV-QOL | 25 | – | 18 |
| Sleep Quality | 8 | – | 4 |
| DASS-Stress | 30 | – | 16 |
| – Depression | 32 | – | 16 |
| – Anxiety | 30 | – | 18 |
| Biochemical variables | |||
| Thyroid profile | |||
| TSH | – | 0.313 | – |
| FREE TRIIODOTHYRONINE (FT3) | 2.41 dl | – | – |
| TRI IODO THYRONINE (T3) | 2.13 ng/mL | – | – |
| THYROXINE (T4) | 21.9 μg/dl | – | – |
| Randomized Blood sugar (RBS) | 93 mg/dl | – | – |
| 75 gm GTT ( Gestational) Fasting | 83 mg/dl | – | – |
| Antenatal scan report | |||
| Right uterine artery PI | 2.89 (positive for PIH) | 1.34 (Negative for PIH) | – |
| Left uterine artery PI | 2.10 (positive for PIH) | 1.59 (Negative for PIH) | – |
| Mean | 2.49 (positive for PIH) | 1.46 (Negative for PIH) | – |
| Obstetric scan | |||
| Fetal biophysical profile Score | |||
| Fetal posture & tone | – | – | Normal –2/2 |
| Fetal movements | – | – | Normal –2/2 |
| Fetal breathing movements | – | – | Normal –2/2 |
| Quantitative amniotic fluid volume | – | – | Normal –2/2 |
| Total BPP Score | – | – | 8/8 |
| Gestational age at Delivery | 36 weeks | ||
| Diagnosis at delivery | Primi 36 weeks with severe PIH | ||
| Mode of delivery | Emergency LSCS under spinal anesthesia | ||
| Sex | Male baby | ||
| Fetal weight | 2.25 kg | ||
| Liquor | Clear | ||
| APGAR score | 8,10 | ||
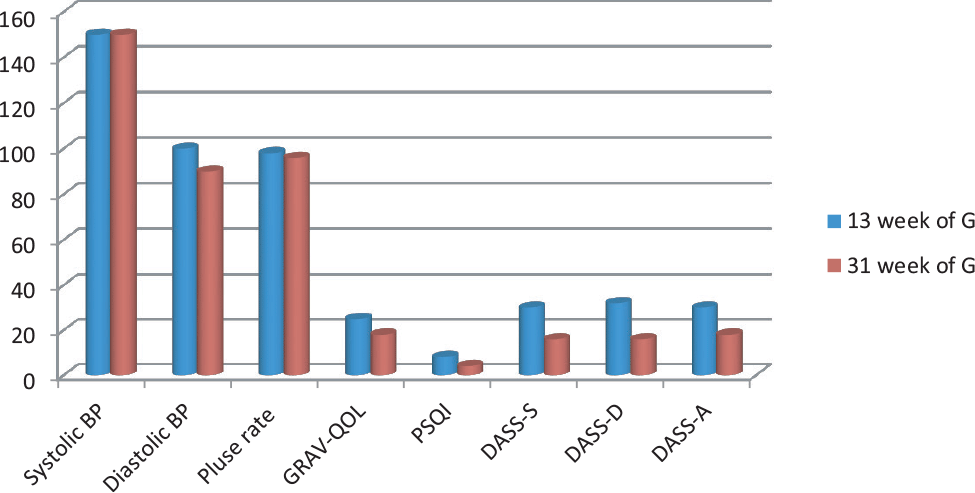
Figure 3: Physiological and Psychological parameters.
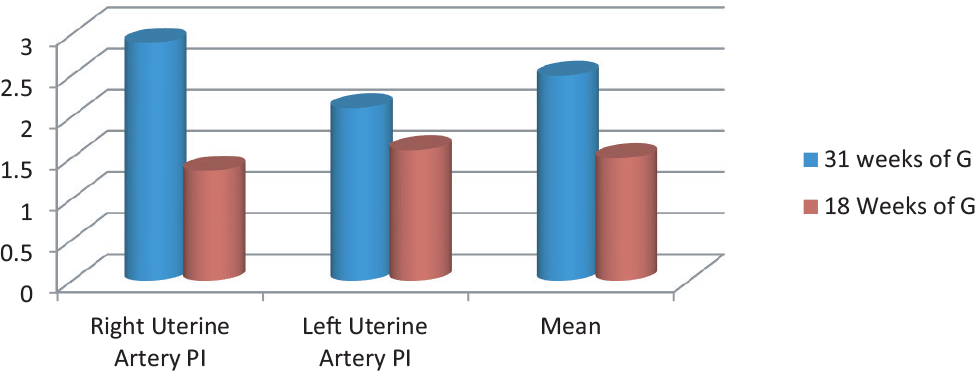
Figure 4: Uterine Artery Doppler.
At 36 weeks of gestational age, obstetric scan, Fetal biophysical profile Score shows a normal range for fetal posture and tone 2/2, Fetal movement 2/2, Fetal breathing movement 2/2, Quantitative amniotic fluid volume 2/2. Each of these five areas has consolidated a score of either 0 (abnormal) or 2 (average).
In total, Biophysical Profile (BPP) is 8/8, which indicates good health of the newborn; newborn weight is around 2.25 kg, and APGAR score is 8, 10, which shows good health since Preterm labour, premature baby, and low APGAR score is the complications of a high-risk pregnancy.
Conclusion
Yoga therapy is effective in managing high-risk pregnancies, such as Pregnancy-induced Hypertension, and Complications of high-risk Pregnancy, such as preterm labour (maternal health), low birth weight, Premature baby, and low APAGR score (Fetal health) in the newborn.
Yoga also impacts improving the quality of life during the gestational period and keeping stable psychological variables on the maternal side, such as anxiety and depression, as well as helping to cope with stress. Yoga is effective as a non-pharmacological treatment without any side effects during a high-risk pregnancy.
Authors’ contribution
RJ, SM, NR: Concept/design of the article, treatment and data acquisition; AK, S, S: Critical analysis and interpretation of data for the article and article-submission.
Informed consent
The study was verbally explained to the patient and written consent was signed by the patient.
Source of funding
None.
Conflict of interest
None.
Received Date: 20-03-23; Revised Date: 06-06-23
Accepted Date: 07-06-23
References
1. Aalami M, Jafarnejad F, Modarres Gharavi M. The effects of progressive muscular relaxation and breathing control technique on blood pressure during pregnancy. Iranian journal of nursing and midwifery research. 2016 May; 21(3):331.
2. Abbaszadeh F, Baghery A, Mehran NA. Quality of life among pregnant women. Hayat. 2009 Mar 1;15(1).
3. Parker SE, Werler MM. Epidemiology of ischemic placental disease: a focus on preterm gestations. In Seminars in perinatology 2014 Apr 1 (Vol. 38, No. 3, pp. 133–138). WB Saunders.
4. Kleebkaow P, Limdumrongchit W, Ratanasiri T, Komwilaisak R, Seejorn K. Prevalence of placental pathology in low birthweight infants. Journal-Medical Association of Thailand. 2006 May 1;89(5):594.
5. Nathan HL, Duhig K, Vousden N, Lawley E, Seed PT, Sandall J, Bellad MB, Brown AC, Chappell LC, Goudar SS, Gidiri MF. Evaluation of a novel device for the management of high blood pressure and shock in pregnancy in low-resource settings: study protocol for a stepped-wedge cluster-randomised controlled trial (CRADLE-3 trial). Trials. 2018 Dec;19(1):1–0.
6. Blencowe H, Cousens S, Oestergaard MZ, Chou D, Moller AB, Narwal R, Adler A, Garcia CV, Rohde S, Say L, Lawn JE. National, regional, and worldwide estimates of preterm birth rates in the year 2010 with time trends since 1990 for selected countries: a systematic analysis and implications. The lancet. 2012 Jun 9;379(9832):2162–72.
7. Altijani N, Carson C, Choudhury SS, Rani A, Sarma UC, Knight M, Nair M. Stillbirth among women in nine states in India: rate and risk factors in study of 886,505 women from the annual health survey. BMJ open. 2018 Nov 1;8(11):e022583.
8. Singh P, Hashmi G, Swain PK. High prevalence of cesarean section births in private sector health facilities-analysis of district level household survey-4 (DLHS-4) of India. BMC public health. 2018 Dec;18(1):1–0.
9. Haruna M, Matsuzaki M, Ota E, Shiraishi M, Hanada N, Mori R. Guided imagery for treating hypertension in pregnancy. Cochrane Database of Systematic Reviews. 2019(4).
10. Maharana S, Nagarathna R, Padmalatha V, Nagendra HR, Hankey A. The effect of integrated yoga on labor outcome: A randomized controlled study. International Journal of Childbirth. 2013 Jan 1;3(3):165–77.
11. Satyapriya M, Nagarathna R, Padmalatha V, Nagendra HR. Effect of integrated yoga on anxiety, depression & well being in normal pregnancy. Complementary therapies in clinical practice. 2013 Nov 1;19(4):230–6.